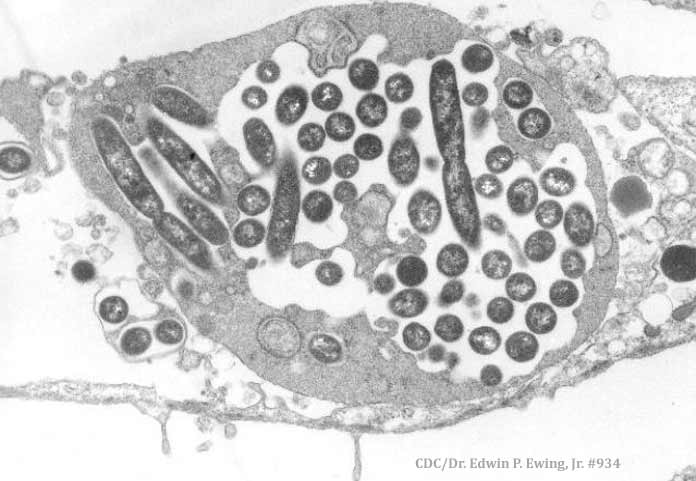
One of the key questions that has arisen from recent revelations regarding the 2014-2015 Legionnaires’ disease outbreak in Flint, Michigan has been whether or not clinical isolates were taken from the 87 people who contracted the illness. Of these 87 victims, 9 died.
Details about the steps that state and county authorities took in their epidemiological investigation of the decade’s largest Legionnaires’ disease outbreak are still emerging as emails from the period are released by Michigan Department of Health and Human Services (MDHHS) and Genesee County Health Department (GCHD) officials.
What seems clear at this point, as discussed below, is that state and county health departments: a) knew early on – in October 2014 – that an outbreak was occurring and that clinical isolates should be collected; but b) failed to acquire the quantity of clinical isolates (despite 42 new Legionnaires’ disease cases that occurred from May 2015 through November 2015) that could definitively connect the outbreak to Flint’s contaminated water supply.
As reported by a set of emails recently released by MDHHS, on October 13, 2014 Shannon Johnson, an infectious disease epidemiologist with Michigan Department of Community Health, alerted DHHS officials to the spike of Legionnaires’ disease cases in Flint. She also recommended that clinical isolates be taken from patients:
“The current hypothesis is that the source of the outbreak may be the Flint municipal water … I let Shurooq [the Genesee County epidemiologist] know that we could assist with and facilitate environmental testing, whether it be through our lab or DEQ [the Department of Environmental Quality]. The LHD [Local Health Department] is meeting with the water dept. this week so she said she would let me know what their plan is. I also requested, again, that she let the area hospitals know if they see any new cases of illness to collect a respiratory culture in addition to the urine antigen test so that if environmental testing is done and Legionella is recovered, there is a clinical sample to compare it to. She let me know that McLaren conducted environmental testing on their system and found low levels of legionella bacteria and have since hyper‐chlorinated their water to disinfect the system. McLaren receives its water from the Flint municipal system.”1
And yet, in its official press release about the Legionnaires’ disease outbreak issued (over a year later) in January 2016, MDHHS announced that the LD cases couldn’t be connected to Flint’s municipal water supply because of the lack of clinical isolates:
“During LD outbreak investigations, clinical specimens are often evaluated against environmental specimens to aid in determining an infection source. One reason that the increase in cases cannot be directly related to the change in Flint water supply is due to the lack of clinical Legionella isolates from case patients. Clinical isolates are necessary to interpret the findings of an environmental investigation in an outbreak.”2
Clinical Isolates Are Essential Pieces of Evidence in Legionnaires Lawsuits
There are 6 key steps in evaluating Legionnaires’ disease claims which we take when formulating legal strategies with our clients:
- We confirm the initial pneumonia diagnosis through radiographic evidence and blood work.
- We confirm that Legionella pneumonia bacteria was found in the patient’s body through clinical isolates (acquired by laboratory testing of urine, blood, respiratory secretions, lung tissue, and pleural fluid).
- We identify possible sources of the illness (where our client was prior to the 2- to 18-day incubation period) and determine whether other Legionnaires’ disease victims were at the same place.
- We review the results of local and state health department epidemiologic investigations.
- We analyze the findings of environmental investigations.
- We look for genetic matches between the bacteria found in patient clinical isolates and environmental samples.
It is thus imperative that, if you or a loved one has contracted Legionnaires’ disease, that you maintain the medical records of clinical isolate testing (typically, urine antigen tests and Polymerase Chain Reaction (PCR) assays of respiratory secretions). Please note: if you think that you may have contracted Legionnaires’ disease within the last six months, this may be verifiable through antibody serology blood tests, which can yield positive results from 3-6 months after infection (sometimes longer). With this key evidence, we can then create a forceful action plan to help you to receive the compensation you are owed.
Our law firm is not taking these cases. Our offices are located in Minneapolis, MN.
Sources:
- Press Release. “MDHHS releases emails related to the Genesee County Legionnaires Disease investigations. Michigan Department of Health and Human Services. Web. 9 Feb. 2016.
- Press Release. “Increased cases of Legionnaires Disease Investigated in Genesee County. Michigan Department of Health and Human Services . Web. Jan. 2016.
- “Summary of Legionellosis Outbreak – Genesee County, June 2014-March 2015.” Michigan Department of Health & Human Services, Communicable Disease Division. 29 May 2015. Web. 9 Feb. 2016.